Research Article - Journal of Environmental and Occupational Health (2022)
Emotional Intelligence and Burnout Among OtorhinolaryngologyâHead and Neck Surgery Residents
Abdulelah M. Sharaf1*, Isra H. Abdulla2, Abdullah M. Alnatheer1, Aghadir N. Alahmari1, Omar A. Alwhibi1, Ziyad Alabduljabbar3 and Feras M. Alkholaiwi32Department of Medicine, Almaarefa University, Riyadh, Saudi Arabia
3Department of Otorhinolaryngology–Head and Neck Surgery, Imam Mohammad Ibn Saud Islamic University, Riyadh, Saudi Arabia
Abdulelah M. Sharaf, Department of Medicine, Imam Mohammad Ibn Saud Islamic University, Riyadh, Saudi Arabia, Email: ams8533@gmail.com
Received: 05-Feb-2022, Manuscript No. JENVOH-22-43915; Editor assigned: 08-Feb-2022, Pre QC No. JENVOH-22-43915 (PQ); Reviewed: 23-Feb-2022, QC No. JENVOH-22-43915; Revised: 28-Feb-2022, Manuscript No. JENVOH-22-43915 (R); Published: 07-Mar-2022
Abstract
Aim: To investigate the relationship between Emotional Intelligence (EI) and burnout among Otorhinolaryngology–Head and Neck surgery residents.
Methods: This cross-sectional study examined 51 residents in different Otorhinolaryngology–Head and Neck surgery programs at different hospitals in Saudi Arabia using a survey conducted from January to March 2021. The questionnaire had different validated measurements of burnout and included the Trait EI Questionnaire- Short Form, the Maslach Burnout Inventory-Human Services survey, and questions regarding demographics and job satisfaction.
Results: Of all residents surveyed, 17.6% had a high risk of burnout, 39.2% had Emotional Exhaustion (EE), 29.4% had Depersonalization (DP), and 43.1% had a low sense of Personal Accomplishment (PA). A statistically significant negative association was observed between total EI score and EE (r= -0.577, p<0.001) and DP (r= -0.765, p<0.001), indicating that higher total EI scores were associated with lower EE levels.
Conclusions: Positive associations existed between high levels of EI, PA, and satisfaction with both surgical skills and specialty choice. Therefore, residency programs should use the EI modifiers as tools to reduce the risk of burnout.
Keywords
Burnout; Emotional intelligence; Otorhinolaryngology-Head and Neck Surgery; ENT; Residents
Introduction
Burnout syndrome is defined as a physiological state characterized and measured by Emotional Exhaustion (EE), Depersonalization (DP), and a low sense of Personal Accomplishment (PA) [1,2]. Burnout can affect anyone regardless of their profession, mostly affecting those with high-demand jobs. Thus, the high-risk group includes health care physicians [3]. Maslach Burnout Inventory (MBI) is a validated measure for burnout evaluation and can be used to develop self-awareness about this issue [1].
The main cause of burnout is the nature of the hospital work; residents and physicians can be affected by the long work hours, lack of sleep, and increase in the number of on-call days. Healthcare providers can be impacted by daily work requirements, such as dealing with breaking bad news to patients or difficult patients [4]. In 2015, a study conducted in Saudi Arabia found a higher incidence of burnout among Otorhinolaryngology–Head and Neck surgery residents in the Saudi Board Training Program compared with other board training programs [5]. An additional study in 2011 found that approximately 41% of Otorhinolaryngology–Head and Neck surgeons showed burnout features [6].
Psychological factors such as Emotional Intelligence (EI) can significantly influence burnout [7]. EI has been defined as “the awareness, control, and expression of one’s emotions and the ability to handle interpersonal relationships judiciously and empathetically” [8]. In 1995, Goleman conceptualized EI as a set of competencies that can be trained and learned [9].
Recently, the medical field has established the potential benefits of EI for the healthcare system [10]. Further, there is increasing interest in the importance of EI in medical training [11]. Moreover, the EI of medical residents and internists is associated with a decreased incidence of burnout and a high degree of job satisfaction [12]. Few studies have examined the association between EI and burnout among surgical residents. A cohort study conducted in the Northeastern United States showed that high EI and positive work experiences were associated with low incidence of burnout among general surgery residents [13]. Other studies have suggested that EI may have a significant impact on a resident’s capability to control the stress factors of training and be useful for optimizing surgical residents’ wellness [14,15]. This study aimed to investigate the relationship between EI and the individual components of burnout among Otorhinolaryngology– Head and Neck surgery residents in Saudi Arabia.
Materials and Methods
We obtained approval from the Institutional Review Board (IRB)/ethics committee of Imam Mohammad ibn Saud Islamic University (IMSIU), Riyadh, Saudi Arabia. A cross-sectional study was conducted on Otorhinolaryngology- Head and Neck Surgery residents (ORL-HNS) registered for different ORL-HNS programs in different hospitals, including university, military, national guard, security forces, and the Ministry of Health hospitals. The survey was conducted from January 2021 to March 2021, and data collectors distributed the survey questionnaires to the residents through social media as well as airdrop. The participants belonged to the R2-R5 program, and received information on the study purpose before obtaining informed consent.
The questionnaire used in the current research included three main parts: demographics, the Trait Emotional Intelligence Questionnaire-Short Form (TEIQueSF), and MBI-Human Services (MBI-HS) survey. Demographics, such as gender and age, were assessed in Part A of the survey. Additional questions were also included to assess job satisfaction, role in the operating room, and job salary, since these variables may affect EI.
EI was assessed using the TEIQueSF, an abbreviated version of the TEIQue. The TEIQueSF includes 30 questions that assess four EI domains: well-being, self-control, sociability, and emotionality. All questions are graded on a scale from 1 (completely disagree) to 7 (completely agree). The overall global score (EI) is calculated by averaging the scores for all 30 items. The survey is scored using an online key (London Psychometric Laboratory). The TEIQue-SF yields a global trait EI score ranging from 1 to 7 and calculated as the mean of the individual question scores. Factor scores also range from 1 to 7. The MBIHS was used to assess the prevalence of various burnout domains among respondents. The MBI-HS survey targets healthcare services and includes 22 questions. The questions assess three domains of burnout: EE (9 questions), sense of PA (8 questions), and DP (5 questions). High scores in the DP and EE domains are associated with a higher risk of burnout. Lower scores in the PA domain are associated with a higher risk of burnout. High EE is identified if the EE score is >26, while high DP is identified if the DP score is >12. A cut-off value of 32 is used to define the PA level. Thus, students with a PA score <32 were classified as having a low sense of PA. The coexistence of high EE and high DP indicated a high risk of burnout.
Statistical analyses were performed using R v 3.6.3. Distributions of continuous variables, EI and burnout dimensions are described using mean ± standard deviation values, and categorical data summarized as counts and percentages. Spearman’s correlation was used to assess the strength and magnitude of the association between the various EI dimensions and burnout. Multiple linear regressions were used for multivariate analysis. Linear regression was used to assess predictors of high EE, low PA, high DP, and EI. Statistical significance was set at p<0.05.
Results
Descriptive statistics
Descriptive statistics of the study sample are provided in Table 1. The questionnaire was completed by 51 Otorhinolaryngology residents (64.7% males and 35.3% females). The average age of the included residents was 27.9 ± 2.1 years. Approximately half of the respondents were married (45.1%). Regarding residency year, half of the respondents were in their second residency year, and 15.7% were in their third. The remaining 17.6% and 17.6% were in their fourth and fifth residency years, respectively. The average weight and height of the included residents were 71.9 kg and 169 cm, respectively. Onethird of the respondents were smokers (31.4%), while the others were non-smokers (68.6%). One-third of the residents reported not doing any exercise, and a quarter reported exercising 2 days/week. Another 23.5% reported exercising for 3 days/week. The mean working hours in the hospital were 13.8 ± 15.4, while the mean number of clinics attended per week was 3.12 ± 1.24. The average number of on-call events per month was 5.54 ± 1.92, while the average number of patients under daily care was 3 ± 2.5. A total of 10 (38.5%) students considered their families supportive, and a similar number thought their families were very supportive.
| Characteristics (N=51) | Value |
|---|---|
| Gender, n (%) | |
| Female | 18 (35.3%) |
| Male | 33 (64.7%) |
| Age (years), mean (SD) | 27.9 (2.14) |
| Current level of residency program, n (%) | |
| R2 | 25 (49.0%) |
| R3 | 8 (15.7%) |
| R4 | 9 (17.6%) |
| R5 | 9 (17.6%) |
| Marital status, n (%) | |
| Married | 23 (45.1%) |
| Not married | 28 (54.9%) |
| Weight (kg), mean (SD) | 71.9 (15.2) |
| Height (cm), mean (SD) | 169 (8.18) |
| Smoker, n (%) | |
| No | 35 (68.6%) |
| Yes | 16 (31.4%) |
| Average numbers of days of exercise/week, n (%) | |
| 0 days | 17 (33.3%) |
| One day | 7 (13.7%) |
| 2 days | 12 (23.5%) |
| 3 days | 12 (23.5%) |
| 4 days | 2 (3.92%) |
| >4 days | 1 (1.96%) |
| Hours of sleep per day, mean (SD) | 6.29 (0.95) |
| Number of on-call events per month, mean (SD) | 5.54 (1.92) |
| Hours/day of working in the hospital, mean (SD) | 13.8 (15.4) |
| Number of clinics attended per week, mean (SD) | 3.12 (1.24) |
| Number of surgeries/week, mean (SD) | 2.81 (1.75) |
| Number of patients under the daily care, mean (SD) | 3.21 (2.50) |
| Spousal support, mean (SD) | |
| Not supportive | 1 (3.85%) |
| Neutral | 5 (19.2%) |
| Supportive | 10 (38.5%) |
| Very supportive | 10 (38.5%) |
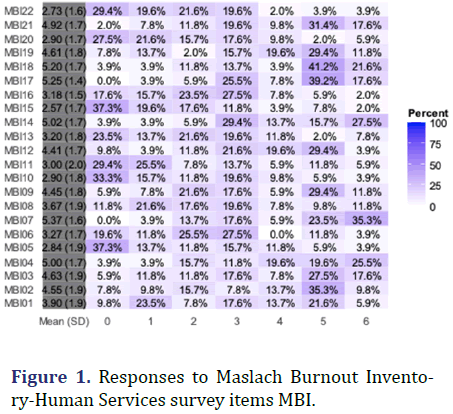
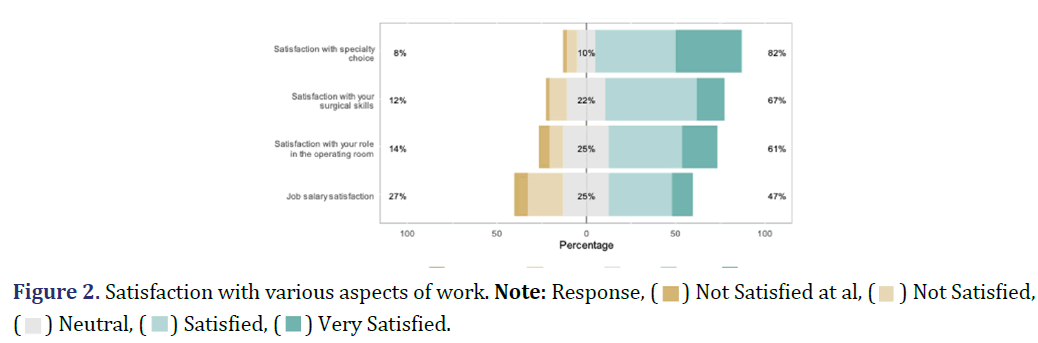
Figure 1 shows the responses to MBI-HS items. About 82% of the residents were satisfied with their specialty choice, while 8% were not satisfied (Figure 2). Further, 67% and 61% of the respondents were satisfied with their surgical skills and roles in the operating room, respectively. Less than half of the residents were satisfied with their job salaries.
The prevalence of EE among Otorhinolaryngology residents was 39.2% (n=20), while the prevalence of DP was 29.4% (n=15). A low sense of PA was observed in 22 (43.1%) residents. Overall, 9 (17.6%) participants had a high risk of burnout (Table 2).
| TEI | Well-being | Self-control | Emotionality | Sociability | EE | DP | PA | |
|---|---|---|---|---|---|---|---|---|
| TEI | 0.814‡ | 0.742‡ | 0.786‡ | 0.824‡ | -0.577‡ | -0.765‡ | 0.680‡ | |
| Well-being | 0.814‡ | 0.508‡ | 0.446† | 0.578‡ | -0.567‡ | -0.570‡ | 0.723‡ | |
| Self-control | 0.742‡ | 0.508‡ | 0.472‡ | 0.507‡ | -0.419† | -0.555‡ | 0.400† | |
| Emotionality | 0.786‡ | 0.446† | 0.472‡ | 0.584‡ | -0.23 | -0.604‡ | 0.369† | |
| Sociability | 0.824‡ | 0.578‡ | 0.507‡ | 0.584‡ | -0.577‡ | -0.688‡ | 0.596‡ | |
| EE | -0.577‡ | -0.567‡ | -0.419† | -0.23 | -0.577‡ | 0.590‡ | -0.613‡ | |
| DP | -0.765‡ | -0.570‡ | -0.555‡ | -0.604‡ | -0.688‡ | 0.590‡ | -0.637‡ | |
| PA | 0.680‡ | 0.723‡ | 0.400† | 0.369† | 0.596‡ | -0.613‡ | -0.637‡ | |
| Note: *p<0.05, †p<0.01, ‡p<0.001. | ||||||||
Correlations between burnout and emotional intelligence
A statistically significant negative association was observed between total EI (TEI) score and EE (r= -0.577, p<0.001) and DP (r= -0.765, p<0.001), indicating that a higher TEI score was associated with lower EE. A higher PA score was associated with a higher TEI score (r=0.68, p<0.001) (Table 3). A statistically significant negative correlation was observed between all EI domains and all MBI-HS domains, except for the association between EE and emotionality (r= -0.23, p>0.05). The correlation between EE and DP was statistically significant (r=0.59, p<0.001). Higher PA scores were associated with lower DP scores (r= -0.637, p<0.001) and EE (r= -0.613, p<0.001). A statistically significant positive correlation was observed between all 4 EI domains, with values ranging from 0.446 to 0.824.
The correlations between burnout domains and EI domains were statistically significant (Table 2). Satisfaction with their skills was significantly associated with TEI score (r=0.4, p<0.05). Similarly, a statistically significant positive association was observed between satisfaction with specialty and TEI score (r=0.31, p<0.05). Satisfaction with salary was not significantly associated with TEI score (r=0.26, p=0.062). No statistically significant association was observed between satisfaction with the role and TEI score (r=0.21, p>0.05).The number of patients under daily care and the number of clinics per week were not significantly correlated with EI, EE, DP, or PA (p>0.05; Table 3). The number of surgeries per week was significantly associated with PA score (r=0.401, p<0.01). The average number of days of exercise/week showed a statistically significant positive correlation with TEI score (r=0.447, p<0.001). The average sleeping hours/ day showed a statistically significant negative correlation with DP (r= -0.277, p<0.05). EE showed a statistically significant positive association with the average number of on-call events/month (r=0.356, p<0.05) and average working hours at the hospital (r=0.324, p<0.05).
A statistically significant negative correlation was observed between satisfaction with salary and EE (r= -0.329, p<0.05) (Table 3). Thus, an increase in satisfaction with salary was associated with a decrease in EE score. Satisfaction with their salary was positively correlated with PA score (r=0.37, p=0.016), while there was a significant negative association between satisfaction with specialty and EE (r= -0.463, p<0.001), between satisfaction with specialty and DP (r= -0.317, p<0.05), and between satisfaction with their role in the operating room with EE (r= -0.414, p<0.01). A statistically significant negative correlation was observed between satisfaction with skills and EE (r= -0.365, p<0.01) as well as between satisfaction with salary and DP (r= -0.29, p<0.05). Two important factors showed a positive association with PA: satisfaction with salary (r=0.37, p<0.01) and satisfaction with specialty choice (r=0.305, p<0.05).
| Variable | EE | DP | PA | TEI |
|---|---|---|---|---|
| Average numbers of days of exercise per week | -0.192 | -0.157 | 0.216 | 0.447† |
| Average hours of sleep per day | -0.118 | -0.277* | 0.072 | 0.232 |
| The average number of on-call events per month | 0.356* | 0.128 | -0.125 | -0.053 |
| Average hours/day of working at the hospital | 0.324* | 0.002 | -0.084 | 0.015 |
| The average number of clinics attended per week | -0.188 | -0.265 | 0.206 | 0.158 |
| The average number of surgeries per week | -0.008 | -0.141 | 0.401† | 0.207 |
| The average number of patients under the daily care | 0.237 | 0.142 | -0.166 | -0.109 |
| Domains of satisfaction | EE | DP | PA | |
| Satisfaction with salary | -0.329* | -0.138 | 0.370† | |
| Satisfaction with specialty | -0.463‡ | -0.317* | 0.305* | |
| Satisfaction with your role in the operating room | -0.414† | -0.234 | 0.188 | |
| Satisfaction with skills | -0.365† | -0.290* | 0.159 | |
| Note: *p<0.05, †p<0.01, ‡p<0.001. | ||||
Linear regression analysis
Age, gender, and residency level were not significantly associated with the TEI score. Marital status did not show a statistically significant association with burnout. The average daily sleeping hours showed a statistically significant association with the TEI score (B=0.026, p<0.05), indicating that one extra sleeping hour is associated with 0.44 units increase in the average EI score. Exercise level also showed a statistically significant association with EI score (B=0.52, p<0.05), indicating that the average EI score was higher by 0.52 in residents who exercise than in those who did not. None of the remaining sociodemographic characteristics were significantly associated with the EI score.
Physical exercise was significantly associated with higher PA scores (B=5.72, p<0.05) (Table 4). Thus, the average PA score increased by 5.72 points in respondents who performed exercises at least once per week compared with those who did not exercise. None of the remaining sociodemographic factors showed statistically significant associations with EE, DP, or PA scores.
| Predictors | Estimates | 95% CI | p | |||
|---|---|---|---|---|---|---|
| Gender: Male vs. Female | -0.21 | -0.59–0.16 | 0.261 | |||
| Age (one-year increase) | 0 | -0.11–0.12 | 0.931 | |||
| Exercise: One day or more vs. Never | 0.52 | 0.15–0.90 | 0.007* | |||
| Residency: R4 to R6 vs. R1 to R3 | 0.38 | -0.12–0.87 | 0.131 | |||
| Average daily sleeping hours: >6 vs. <6 | 0.44 | 0.05–0.82 | 0.026* | |||
| Smoker: Yes vs. No | 0 | -0.37–0.37 | 0.986 | |||
| Marital status: Not married vs. Married | -0.24 | -0.60–0.12 | 0.189 | |||
| Predictors | EE | DP | PA | |||
| Estimates | p | Estimates | p | Estimates | p | |
| (95% CI) | (95% CI) | (95% CI) | ||||
| (Intercept) | 38.37 | 0.237 | 9.06 | 0.584 | 3.76 | 0.855 |
| (-26.22–102.97) | (-24.02–42.15) | (-37.40–44.92) | ||||
| Gender: Male vs. Female | -4.73 | 0.219 | 2.58 | 0.191 | -3.04 | 0.216 |
| (-12.38–2.92) | (-1.34–6.50) | (-7.91–1.84) | ||||
| Age (one-year increase) | -0.07 | 0.95 | 0.05 | 0.928 | 0.88 | 0.241 |
| (-2.41–2.27) | (-1.14–1.25) | (-0.61–2.37) | ||||
| Exercise: One day or more vs. Never | -6.1 | 0.115 | -0.74 | 0.706 | 5.72 | 0.022* |
| (-13.74–1.54) | (-4.65–3.18) | (0.85–10.59) | ||||
| Residency: R4 to R6 vs. R1 to R3 | -8.34 | 0.101 | -4.6 | 0.078 | 0.4 | 0.899 |
| (-18.38–1.70) | (-9.74–0.54) | (-5.99–6.80) | ||||
| Average daily sleeping hours: >6 vs. <6 | -0.03 | 0.993 | -3.59 | 0.078 | 2.76 | 0.271 |
| (-7.85–7.79) | (-7.59–0.42) | (-2.23–7.74) | ||||
| Smoker: Yes vs. No | 2.14 | 0.572 | -0.29 | 0.88 | 3.6 | 0.14 |
| (-5.43–9.71) | (-4.17–3.59) | (-1.23–8.42) | ||||
| Marital status: Not married vs. Married | -2.92 | 0.434 | 3.05 | 0.114 | -4.03 | 0.094 |
| (-10.37–4.53) | (-0.76–6.87) | (-8.78–0.71) | ||||
| Note: *p<0.05. | ||||||
Discussion
Among 684 Otorhinolaryngology residents in the United States, a high burnout rate was reported in 10% and a moderate rate in 76%; in our study, 17.6% of residents were at high risk of burnout, a valuable statistic despite the small sample size of 51 participants. Residency training is arguably the most important and difficult period of a medical career, physicians are required to improve their character and hone their skills as they become more knowledgeable in their fields while carrying out a daily workload considered being heavier than that at higher career levels. Those years of training can affect residents physically and psychologically. The high prevalence of burnout among residents in general and surgical residency training is especially alarming [16], and despite a plethora of recent research papers on the magnitude of burnout and its consequences, research on the individualistic factors affecting the tendency for burnout and how to deal with them is still lacking.
There are many causes for burnout that cannot be controlled or avoided, which makes understanding those that can be controlled or improved more valuable. Studies on the significance of personality traits in predicting burnout have shown contradictory results. Therefore, personality traits may not have a consistently reliable predictive relationship with burnout [6-13]. EI, comprising well-being, self-control, sociability, and emotionality, was found to have a significant relation to the propensity of burnout among physicians in a handful of studies [17]. Therefore, EI assessment can be employed as a tool to better understand the individualistic experiences of residents regarding burnout, factors that make them more vulnerable, and protective factors. It also suggests EI assessment as a strategic tool for lowering the risk of burnout better than advising residents to undergo mental health counseling, especially since the constituents of EI are modifiable [13].
In a meta-analysis of studies that measured burnout prevalence using the MBI, the international prevalence rate of burnout among surgical residents was 51%. In the United States, the prevalence rate of burnout among residents was found to range from 27% to 75% according to specialty [18], and a study focused on surgical specialties found that when applying the strict scales of EE, DP, and PA, 3% of the participants were found to have burnout syndrome, and upon individually evaluating the subscales od burnout syndrome, the percentage of affected participants increased to 50, with high EE or DP in one out of every three surgeons [19].
In our study, high EI scores were associated with lower EE scores, indicating that residents with high EI were better equipped to avoid EE, which represents the stress dimension of burnout syndrome that leads to the affected individuals distancing themselves from work both cognitively and emotionally [20]. High EE scores were positively associated with a higher average number of on-call events per month and higher average working hours and negatively associated with satisfaction in both salary and role in the operating theater. Thus, it is plausible to theorize that EE corresponds to the workload and decreases with improvement in efficacy and rewards. Similarly, DP, representing the cynical aspect of burnout, was strongly associated with EE, and therefore, negatively correlated with EI. These findings confirm the importance of allowing for tolerable working hours, as physical and mental exhaustion translates to EE, and the need for integration of operating theater roles from the beginning of the residency program should be examined as it reflects lower EE levels.
The EI score positively correlated with a sense of PA and satisfaction with both surgical skills and specialty choice. As high EI increases the ability to manage stress and decreases the chances of experiencing EE [20], it is possible that a satisfactory job experience, sense of accomplishment, and satisfaction with the own skills are easier to achieve for those with high EI traits.
Some key findings highlighted the importance of residents’ lifestyles, suggesting that lifestyle modifications could be used to increase EI levels, which could further help to deal with different domains of burnout syndrome and reduce its risk. Both average daily sleeping hours and physical exercise were positively correlated with TEI scores, and in the burnout domains, higher PA scores positively correlated with physical exercise.
Tolerable working hours, fair pay, and safe assignment of operating theater roles to residents have been shown to decrease EE and thereby enhance EI. Physical exercise increases the sense of PA, and together with sufficient sleeping hours, it reflects higher EI levels. All these aspects can be targeted to enhance EI and reduce the risk of burnout. Further research on EI factors and their relationship to burnout needs to be conducted in various specialties, and a detailed framework to enhance modifiable EI constituents as a way of decreasing the risk of burnout needs to be considered.
Our study reflects the participants’ subjective perspectives. However, their work performance was not evaluated to confirm the positive or negative effects of higher or lower EI levels, making it a possible limitation. Moreover, the relatively small sample size might have led to non-response bias.
Conclusion
The present study demonstrated a high risk of burnout among surgical specialty residents. Residents with higher EI levels had a lower risk of burnout. EI factors can be modified and enhanced, for instance, by lifestyle modifications. Residency programs can benefit from EI measurements for estimating the risk of burnout and integrate EI modifiers to reduce the high risk of burnout.
Acknowledgments
We are thankful to Dr. Sulaiman Al Habib Medical Group’s Research Center for their tremendous support.
Funding
This research received no external funding
Conflict of Interest Statement
Authors have no conflict of interest and did not receive any financial funding for this work.
References
- Maslach C, Jackson SE, Leiter MP. Maslach Burnout Inventory: Third edition. Evaluating stress: A book of resources 1997;191–218.
- Bianchi R, Schonfeld IS, Laurent E. Is it time to consider the “burnout syndrome” a distinct illness? Front Public Health 2015;3:158.
[Crossref] [Google scholar] [Pubmed]
- Kumar S. Burnout and doctors: prevalence, prevention and intervention. Healthcare [Basel] 2016;4:37.
[Crossref] [Google scholar] [Pubmed]
- Alotaibi AK, Alsalim A, Alruwaili F, Almubarak A, Alhamzah A, Albahlal A, et al. Burnout during ophthalmology residency training: a national survey in Saudi Arabia. Saudi J Ophthalmol 2019;33:130-134.
[Crossref] [Google scholar] [Pubmed]
- Aldrees T, Badri M, Islam T, Alqahtani K. Burnout among otolaryngology residents in Saudi Arabia: a multicenter study. J Surg Educ 2015;72:844-848.
[Crossref] [Google scholar] [Pubmed]
- Balch CM, Shanafelt TD, Sloan JA, Satele DV, Freischlag JA. Distress and career satisfaction among 14 surgical specialties, comparing academic and private practice settings. Ann Surg 2011;254:558-568.
[Crossref] [Google scholar] [Pubmed]
- Galaiya R, Kinross J, Arulampalam T. Factors associated with burnout syndrome in surgeons: a systematic review. Ann R Coll Surg Engl 2020;102: 401-407.
[Crossref] [Google scholar] [Pubmed]
- Salovey P, Mayer JD. Emotional intelligence. Imagination, cognition and personality 1990;9:185-211.
- Bhoumick P. It's really matter: review of the book, Emotional Intelligence: why it can matter more than IQ’ by Daniel Goleman. Research Journal of Humanities and Social Sciences 2018;9:639-644.
- Sharp G, Bourke L, Rickard M. Review of emotional intelligence in health care: an introduction to emotional intelligence for surgeons. ANZ J Surg 2020;90:433-440.
[Crossref] [Google scholar] [Pubmed]
- McKinley SK, Phitayakorn R. Emotional intelligence and simulation. Surg Clin North Am 2015;95:855-867.
[Crossref] [Google scholar] [Pubmed]
- Weng HC, Hung CM, Liu YT, Cheng YJ, Yen CY, Chang CC, et al. Associations between emotional intelligence and doctor burnout, job satisfaction, and patient satisfaction. Med Educ 2011;45:835-842.
[Crossref] [Google scholar] [Pubmed]
- Lindeman B, Petrusa E, McKinley S, Hashimoto DA, Gee D, Smink DS, et al. Corrigendum to “Association of burnout with emotional intelligence and personality in surgical residents: Can we predict who is most at risk?” [J Surg Educ [2017] e22-e30]. J Surg Educ 2018;75:1135-1146.
[Crossref] [Google scholar] [Pubmed]
- Cofer KD, Hollis RH, Goss L, Morris MS, Porterfield JR, Chu DI. Burnout is associated with emotional intelligence but not traditional job performance measurements in surgical residents. J Surg Educ 2018;75:1171-1179.
[Crossref] [Google scholar] [Pubmed]
- Lin DT, Liebert CA, Tran J, Lau JN, Salles A. Emotional intelligence as a predictor of resident well-being. J Am Coll Surg 2016;223:352-358.
[Crossref] [Google scholar] [Pubmed]
- Serenari M, Cucchetti A, Russo PM, Fallani G, Mattarozzi K, Pinna AD, et al. Burnout and psychological distress between surgical and non-surgical residents. Updates Surg 2019;71:323-330.
[Crossref] [Google scholar] [Pubmed]
- Dahmash A, Alhadlaq AS, Alhujayri AK, Alkholaiwi F, Alosaimi NA. Emotional intelligence and burnout in plastic surgery residents: is there a relationship? Plast Reconstr Surg Glob open 2019;7:e2057.
[Crossref] [Google scholar] [Pubmed]
- Martini S, Arfken CL, Churchill A, Balon R. Burnout comparison among residents in different medical specialties. Acad Psychiatry 2004;28:240-242.
[Crossref] [Google scholar] [Pubmed]
- Bartholomew AJ, Houk AK, Pulcrano M, Shara NM, Kwagyan J, Jackson PG, et al. Meta-analysis of surgeon burnout syndrome and specialty differences. J Surg Educ 2018;75:1256-1263.
[Crossref] [Google scholar] [Pubmed]
- Maslach C, Schaufeli WB, Leiter MP. Job burnout. Annu Rev Psychol 2001;52:397-422.
[Crossref] [Google scholar] [Pubmed]
Copyright: © 2022 The Authors. This is an open access article under the terms of the Creative Commons Attribution NonCommercial ShareAlike 4.0 (https://creativecommons.org/licenses/by-nc-sa/4.0/). This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.






 ) Not Satisfied at al, (
) Not Satisfied at al, ( ) Not Satisfied,
(
) Not Satisfied,
( ) Neutral, (
) Neutral, ( ) Satisfied, (
) Satisfied, ( ) Very Satisfied.
) Very Satisfied.